كتاب fluid therapy
fluid therapy من كتب طب Fluid replacement or fluid resuscitation is the medical practice of replenishing bodily fluid lost through sweating, bleeding, fluid shifts or other pathologic processes. Fluid replacement Cholera rehydration nurses.jpg A person with cholera drinking oral rehydration solution (ORS) [edit on Wikidata] Fluid replacement or fluid resuscitation is the medical practice of replenishing bodily fluid lost through sweating, bleeding, fluid shifts or other pathologic processes. Fluids can be replaced with oral rehydration therapy (drinking), intravenous therapy, rectally such as with a Murphy drip, or by hypodermoclysis, the direct injection of fluid into the subcutaneous tissue. Fluids administered by the oral and hypodermic routes are absorbed more slowly than those given intravenously-
من كتب الطب البشري - مكتبة كتب الطب.

قراءة كتاب fluid therapy أونلاين
معلومات عن كتاب fluid therapy:
Fluid replacement or fluid resuscitation is the medical practice of replenishing bodily fluid lost through sweating, bleeding, fluid shifts or other pathologic processes.
Fluid replacement
Cholera rehydration nurses.jpg
A person with cholera drinking oral rehydration solution (ORS)
[edit on Wikidata]
Fluid replacement or fluid resuscitation is the medical practice of replenishing bodily fluid lost through sweating, bleeding, fluid shifts or other pathologic processes. Fluids can be replaced with oral rehydration therapy (drinking), intravenous therapy, rectally such as with a Murphy drip, or by hypodermoclysis, the direct injection of fluid into the subcutaneous tissue. Fluids administered by the oral and hypodermic routes are absorbed more slowly than those given intravenously
عدد مرات التحميل : 19784 مرّة / مرات.
تم اضافته في : الجمعة , 25 مارس 2016م.
حجم الكتاب عند التحميل : 9.5 كيلوبايت .
تعليقات ومناقشات حول الكتاب:
العلاج بالسوائل من كتب طب بيطرى
العلاج بالسوائل من كتب طب
استبدال السوائل أو إنعاش السوائل هو الممارسة الطبية لتجديد السوائل الجسدية المفقودة من خلال التعرق أو النزيف أو تحولات السوائل أو العمليات المرضية الأخرى.
استبدال السوائل
Cholera rehydration nurses.jpg
الشخص المصاب بالكوليرا يشرب محلول معالجة الجفاف عن طريق الفم (ORS)
[عدل في ويكي بيانات] إن
استبدال السوائل أو إنعاش السوائل هو الممارسة الطبية لتجديد سوائل الجسم المفقودة من خلال التعرق أو النزيف أو تغير السوائل أو غيرها من العمليات المرضية. يمكن استبدال السوائل بعلاج معالجة الجفاف عن طريق الفم (الشرب) ، أو العلاج عن طريق الوريد ، أو عن طريق المستقيم مثل بالتنقيط المورفي ، أو عن طريق الحقن المباشر للسائل في الأنسجة تحت الجلد. يتم امتصاص السوائل التي يتم تناولها عن طريق الفم والطرق تحت الجلد بشكل أبطأ من تلك التي تُعطى عن طريق الوريد
يحتاج المرضى في المستشفى إلى سوائل وريدية (IV) وشوارد لواحد أو أكثر من الأسباب التالية (4Rs):
Fluid resuscitation
IV fluids may need to be given urgently to restore circulation to vital organs following loss of intravascular volume due to bleeding, plasma loss, or excessive external fluid and electrolyte loss, usually from the gastrointestinal (GI) tract, or severe internal losses (e.g. from fluid redistribution in sepsis).
Routine maintenance
IV fluids are sometimes needed for patients who simply cannot meet their normal fluid or electrolyte needs by oral or enteral routes but who are otherwise well in terms of fluid and electrolyte balance and handling i.e. they are essentially euvolaemic, with no significant deficits, ongoing abnormal losses or redistribution issues. However, even when prescribing IV fluids for more complex cases, there is still a need to meet the patient’s routine maintenance requirements, adjusting the maintenance prescription to account for the more complex fluid or electrolyte problems. Estimates of routine maintenance requirements are therefore essential for all patients on continuing IV fluid therapy.
Replacement
In some patients, IV fluids to treat losses from intravascular and or other fluid compartments, are not needed urgently for resuscitation, but are still required to correct existing water and/or electrolyte deficits or ongoing external losses. These losses are usually from the GI or urinary tract, although high insensible losses occur with fever, and burns patients can lose high volumes of what is effectively plasma. Sometimes, these deficits have developed slowly with associated compensatory adaptations of tissue electrolyte and fluid distribution that must be taken into account in subsequent replacement regimens (e.g. cautious, slow replacement to reduce risks of pontine demyelinosis).
Redistribution
In addition to external fluid and electrolyte losses, some hospital patients have marked internal fluid distribution changes or abnormal fluid handling. This type of problem is seen particularly in those who are septic, otherwise critically ill, post-major surgery or those with major cardiac, liver or renal co-morbidity. Many of these patients develop oedema from sodium and water excess and some sequester fluids in the GI tract or thoracic/peritoneal cavities.
Deciding on the optimal amount, composition and rate of administration of IV fluids to address these often complex needs is inherently difficult yet assessment, prescribing and monitoring of IV fluids in general admission and ward areas of hospitals, is often left to junior doctors and hard-pressed nurses who may lack required training and competence.56,57,86,87,93 Evidence suggests that mismanagement of fluids is common, particularly in general ward areas with the potential for adverse outcomes including excess morbidity and mortality, prolonged hospital stays and increased costs.6,39,73,105,116,117
There is, therefore, a clear need for guidance on IV fluid prescribing applicable to general ward areas but since most randomized controlled trials of IV fluid therapy have examined narrow clinical questions in intensive care or intra-operative settings, many recommendations for more general use must be based on first principles. All health professionals involved in prescribing and administering IV fluids need to understand these principles if they are to prescribe and manage IV fluid therapy safely and effectively.
Go to:
5.1. The principles of fluid prescribingb
The knowledge needed to underpin safe and effective IV fluid and electrolyte prescribing lies in four areas:
The physiology of fluid balance in health;
Pathophysiological effects on fluid balance;
Clinical approaches to assessing IV fluid needs;
The properties of available IV fluids.
5.1.1. The physiology of fluid balance in health
When primitive marine unicellular organisms evolved into multicellular organisms and emerged onto land, they carried with them their own internal sea or extracellular fluid (ECF), in which their cells could bathe in a constant chemical environment. The French physiologist Claude Bernard called this the ‘milieu interieur’, 10 an environment in which the cells retain their energy consuming capacity to pump sodium out and retain potassium in order to neutralise the negative charges of proteins and other ions.
While fluid balance is usually considered as that between the body and its environment, i.e. external balance, disease also affects the internal balance between the various body fluid compartments, e.g. between the intravascular and interstitial components of the extracellular fluid compartment (ECF), between the intracellular fluid (ICF) and the ECF, and between the ECF and the gut and other internal spaces.58,60 Appropriate IV fluid therapy depends on an understanding of the underlying physiology and pathophysiology and a consideration not only of external but internal fluid balance.58
5.1.1.1. Normal anatomy and physiology
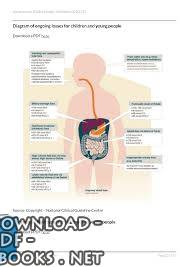
Water comprises approximately 60% of the body weight of an average adult (about 40L in a 70kg man).29 The percentage is lower in obesity, since adipose tissue contains less water than lean tissue. It is also lower in women than in males because of the relatively greater amount of adipose tissue in women. The total body water is divided functionally into the extracellular (ECF=20% of body weight, about 14L in a 70kg man ) and the intracellular fluid spaces (ICF= 40% of body weight, about 28L in a 70kg man) separated by the cell membrane with its active sodium pump, which ensures that sodium remains mainly in the ECF. The cell, however, contains large anions such as protein and glycogen, which cannot escape and, therefore, draw in K+ ions to maintain electrical neutrality (Gibbs-Donnan equilibrium). These mechanisms ensure that Na+ and its balancing anions, Cl- and HCO3-, are the mainstay of ECF osmolality, and K+ has the corresponding function in the ICF. The ECF is further divided into the intravascular (within the circulation) and the interstitial (extravascular fluid surrounding the cells) fluid spaces. The intravascular space (blood volume = 5–7% of body weight, approx. 4 – 5L) has its own intracellular component in the form of red (haematocrit = 40–45%) and white cells and an extracellular element in the form of plasma (55–60% of total blood volume). The normal distribution of fluids in the different body compartments is shown in Figure 2 which also shows the likely compartmental distribution of some different types of IV fluids (see section 5.1.4).
الشكل 2. حجرات ماء الجسم وتوزيع تقريبي للسوائل الوريدية شائعة الاستخدام.
العلاج
بالسوائل العلاج بالسوائل pdf
نوع العلاج بالسوائل
إرشادات العلاج بالسوائل الوريدية
العلاج بالسوائل جزء لكل تريليون
حساب العلاج ببدائل السوائل
أنواع السوائل IV
العلاج بالسوائل
3 أنواع رئيسية من السوائل الوريدية
 مهلاً !
مهلاً !قبل تحميل الكتاب .. يجب ان يتوفر لديكم برنامج تشغيل وقراءة ملفات pdf
يمكن تحميلة من هنا 'تحميل البرنامج'

نوع الكتاب : pdf.
اذا اعجبك الكتاب فضلاً اضغط على أعجبني و يمكنك تحميله من هنا:


كتب اخرى في كتب الطب البشري

2. Treatment of potassium balance disorders PDF
قراءة و تحميل كتاب 2. Treatment of potassium balance disorders PDF مجانا

Laboratory Exercises Microbiology ( second edition) PDF
قراءة و تحميل كتاب Laboratory Exercises Microbiology ( second edition) PDF مجانا